












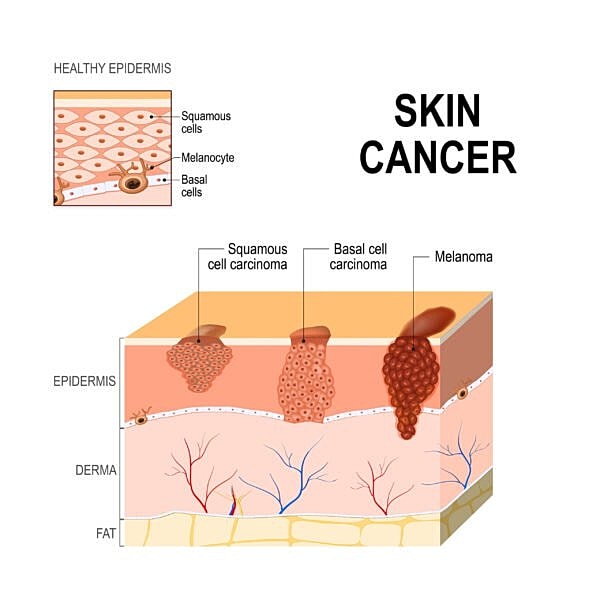
There are three major skin cancer types. Basal cell carcinoma, squamous cell carcinoma and malignant melanoma. Of these three, malignant melanoma is considered the most serious form of skin cancer. This is because there is a higher likelihood of metastasis or spreading of disease throughout the body. In general, early stage melanomas such as stage 1 have good outcomes. Later stages, such as stage 4 are more likely to have metastasis.
There are four major types of malignant melanoma including superficial spreading, nodular melanoma, lentigo maligna melanoma, and acral (hands, feet, ears, nose) melanoma.
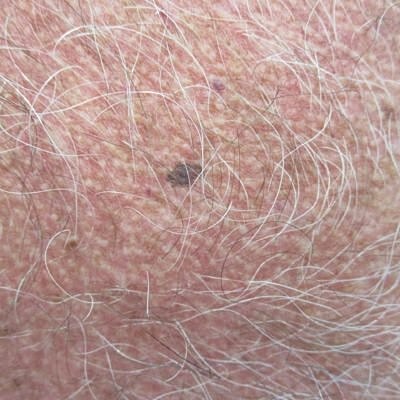
The most common of the four types of malignant melanoma is superficial spreading. Upwards of 70 percent of all melanomas fall into this category and that tends to be a good thing. The majority of superficial spreading melanomas are exactly that; superficial. This tends to mean the skin cancer is thinner or the tumor thickness is less than 1 mm. Tumor thickness is extremely important when diagnosed with melanoma as the thicker the tumor the harder it is to cure and the higher chances of metastasis. With superficial spreading melanoma the majority of cases are curable.
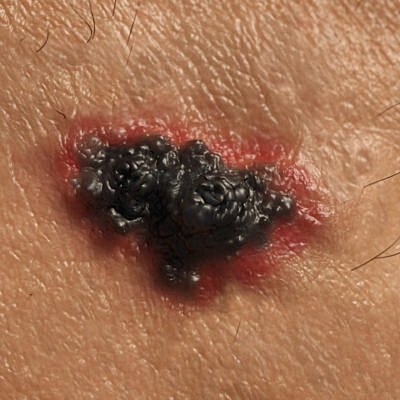
Next up is nodular melanoma and this is the second most common type of melanoma after superficial spreading. Compared to superficial spreading melanoma this type of tumor tends to be thicker. Most nodular melanoma are twice the depth of superficial spreading melanomas, 2 mm. That doesn’t seem like a big deal, but the skin is not very thick. So, 2 mm is actually quite deep.
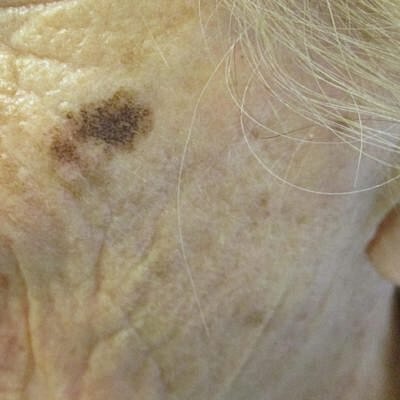
Lentigo maligna melanoma we tend to see in older patients in areas on skin that has had long term sun exposure. This means areas like the face and chest. These tend to be slow growing tumors that may develop over the course of years when compared to other melanomas that may seem to appear out of nowhere.
Lastly, acral melanoma, those that tend to appear on the peripheral areas of our body is the least common. As compared to fair skinned individuals, this type tends to affect those with darker complexions. These are typically found on the hands and feet or even in the nailbeds.
Cumulative sun exposure from the beach, boat, tanning beds, etc. is the most obvious risk factor for developing a melanoma. However, there are numerous other factors that may contribute to the development of this deadly skin cancer. Fair skin, light eyes, having numerous dark moles on your body, family history of melanoma, and even being immunosuppressed by certain medications or disease processes. Keep in mind that although existing moles can transform into melanoma the vast majority of melanomas are new spots. So always be on the lookout for the “ugly duckling”, which is the new mole that does not look like any other mole on your body!


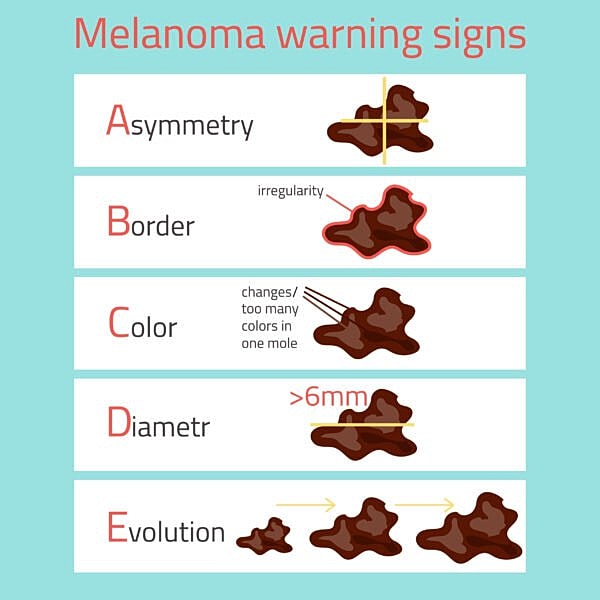
Melanoma is not always easy to identify in its early stages. The best thing to do is once per month look over your skin, preferably with the help of someone for areas that are hard to observe such as your back. Follow the ABCDE rule and if you notice something that doesn’t look right make an appointment to be seen as soon as possible.
A stands for asymmetry. This simply means that if you draw a line down the middle of the mole the two halves are not identical.
B stands or border irregularity. You are looking for borders that are jagged or do not look like your other moles.
C stand for color changes. Do you have dozens or brown or black moles, but one looks like it has other colors in it like red, blue, or even white? Those are the types of color changes you should be on the lookout for.
D stands for diameter. Although not a hard and fast rule, the majority of melanomas tend to be 6 mm or larger. That’s about the size of a pencil eraser.
E stands for evolving or evolution. In my opinion this is the most important. I like to call it “ever changing”. If you notice a mole that is changing size, shape, color, texture, is bleeding, or just does not “look right”; it’s time to be seen in the office.

Treatment for melanomas include surgical excision with wide safety margins. In addition to surgery some patient may need to undergo further treatment with chemotherapy, radiation, immunotherapy or even a combination of therapies.
Tumor staging is one of the most important prognostic factors when being diagnosed with malignant melanoma. Although all cases of melanoma and patients are unique, this gives a general guideline of what to expect in regards to outcomes. Melanoma has four stages where the higher the staging the worse the prognosis. Depending on the stage of melanoma and the tumor thickness additional tests may be ordered. For example, a tumor that is 1.1 mm thick would require a sentinel lymph node biopsy and PET/CT scans. This is to help determine if the tumor has spread to other parts of the body. Thankfully, melanoma research and treatments are getting better and better. The five-year survival rate for melanoma overall is around 91%; and those with localized disease (not spreading) can be as high as 98%.

The American Cancer Society provides the following information regarding survival rates for melanoma by stages. Please remember that all patients and all tumors are unique. These are overall and generalized survival rates.
Stage IA: The 5-year survival rate is around 97%. The 10-year survival is around 95%.
Stage IB: The 5-year survival rate is around 92%. The 10-year survival is around 86%.
Stage IIA: The 5-year survival rate is around 81%. The 10-year survival is around 67%.
Stage IIB: The 5-year survival rate is around 70%. The 10-year survival is around 57%.
Stage IIC: The 5-year survival rate is around 53%. The 10-year survival is around 40%.
Stage IIIA: The 5-year survival rate is around 78%. The 10-year survival is around 68%.*
Stage IIIB: The 5-year survival rate is around 59%. The 10-year survival is around 43%.
Stage IIIC: The 5-year survival rate is around 40%. The 10-year survival is around 24%.
Stage IV: The 5-year survival rate is about 15% to 20%. The 10-year survival is about 10% to 15%. The outlook is better if the spread is only to distant parts of the skin or distant lymph nodes rather than to other organs, and if the blood level of lactate dehydrogenase (LDH) is normal
*The survival rate is higher for stage IIIA cancers than for some stage II cancers. This is likely because the main (primary) tumor is often less advanced for IIIA cancers, although this is not clear.
There’s med spas, and then there’s Ocean Drive Med Spa. Led by Dr. Alan Durkin, Ocean Drive Med Spa is well known among industry professionals as a center for innovation.
Pioneering new technologies and treatments, Ocean Drive Med Spa constantly researches new technologies to ensure the best results for its patients. Ocean Drive Med Spa also features one of the largest laser and energy centers in the nation, offering patients treatments with the latest state-of-the-art tools to create incredible aesthetic experiences. Begin yours today with an appointment at Ocean Drive Med Spa.