












Early-stage skin cancer is highly curable. The team at Ocean Drive Dermatology & Plastic Surgery, located in Indian River Shores and Vero Beach, FL, diagnoses skin cancer early with annually cancer screenings, available to patients throughout the greater Treasure Coast area.
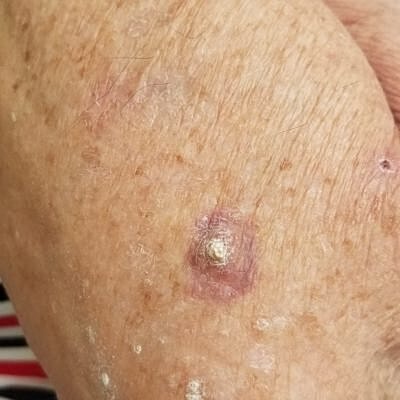
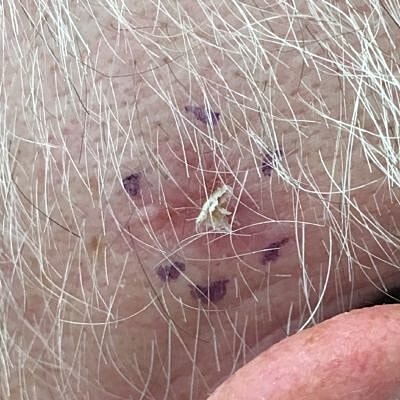
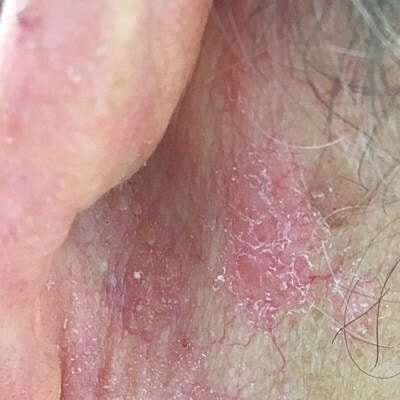
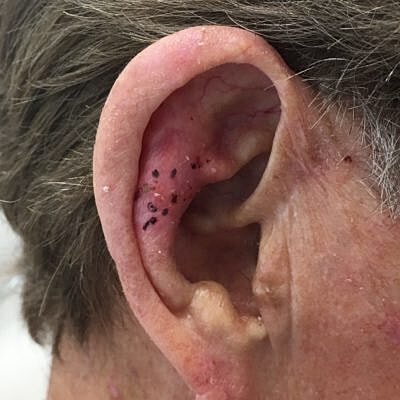
Squamous cell carcinoma (SCC) is a very common type of skin cancer that can occur anywhere on the body that has had too much sun. In fact, it is the second most common with about one million diagnosed each year. Just like other skin cancers, those with fair skin and long-term sun exposure are at greater of developing one. Also, not surprisingly, we tend to see SCC in older patients as it takes time for the cumulative effects of the ultraviolet exposure to take its toll. With that said, it’s not unheard of for someone under 40 to be diagnosed with a SCC, especially in southern Florida and those with a history of using a tanning bed. The most common location to develop a SCC is on the head or neck.
Although we tend to refer to a squamous cell skin cancer as a squamous cell skin cancer there are actually some sub-types of SCC. Squamous cell carcinoma in-situ, SCC-IS, Bowen’s Disease. These are all the same thing. Basically, SCC-IS means that the skin cancer only involves the outermost layer of skin called the epidermis and has not gone into the second layer of skin called the dermis.
Invasive SCC. When people hear the word invasive they tend to think it means the SCC had spread to other parts of the body. This is not typically the case. In fact, it is rare that a squamous cell skin cancer would spread beyond the skin. We think the number is between two and five percent of SCC spread. Invasive SCC goes past the epidermis and into the dermal layer of skin; sometimes even to deeper structures of the skin.

Keratoacanthoma or KA. Although this does not have squamous cell in the name we tend to lump this in the same category because it resembles and acts like SCC. In fact, when looking at a KA under the microscope it’s not always easy to tell the difference between it and an SCC, thus why we typically put it in the same category as SCC.
There are several treatment options for SCC based on location of the skin cancer (face vs back) and type (SCC-IS vs invasive). Treatment could include surgical excision, Mohs micrographic surgery, electrosurgery (ED&C, electrodesiccation and curettage), radiation therapy, and topical therapies such as fluorouracil (Efudex). The prognosis for SCC is very good.
Once the skin cancer is removed or otherwise treated it is extremely important to have good follow up. Like all cancer, skin cancer can recur in the same treated area or develop in a new area. We recommend a total body skin exam every six months for two years after the diagnosis of a squamous cell skin cancer. If no other skin cancers are found during that time period we then recommend yearly total body skin examinations. Possibly more important is the need to look over your body once a month at home. Trust your instincts. If a spot does not heal, bleeds, or somehow is different from your other moles you should come in for an office visit sooner.
There’s med spas, and then there’s Ocean Drive Med Spa. Led by Dr. Alan Durkin, Ocean Drive Med Spa is well known among industry professionals as a center for innovation.
Pioneering new technologies and treatments, Ocean Drive Med Spa constantly researches new technologies to ensure the best results for its patients. Ocean Drive Med Spa also features one of the largest laser and energy centers in the nation, offering patients treatments with the latest state-of-the-art tools to create incredible aesthetic experiences. Begin yours today with an appointment at Ocean Drive Med Spa.